Topline results from Phase II study of SHP607 in extremely premature infants
Posted: 30 June 2016 | | No comments yet
While the study did not meet its primary endpoint of reducing severity of ROP, it did produce encouraging secondary endpoints related to lung and brain…
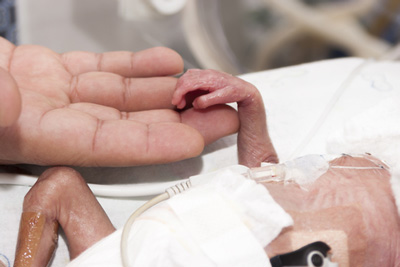

Shire’s Phase II study evaluating an investigational protein replacement, SHP607, in extremely premature infants did not meet its primary endpoint of reducing the severity of retinopathy of prematurity (ROP).


The study, however, demonstrated clinically relevant effects in secondary endpoints related to the development of severe bronchopulmonary dysplasia (BPD), a chronic lung disease, and severe intraventricular haemorrhage (IVH), a type of brain injury, both of which have lifelong negative implications for normal development.
SHP607 is a recombinant human version of the naturally-occurring protein complex of insulin-like growth factor 1 (IGF-1) and its most abundant binding protein, IGF binding protein-3 (IGFBP-3).
The Phase II study included 121 extremely premature infants (born between 23 weeks and 27 weeks +6 days) randomised at birth to either SHP607 or standard neonatal care, and treated continuously until an equivalent gestational age of 30 weeks. IGF-1 is a growth factor that plays a major role in the development of the growing foetus in the uterus. It is supplied by the mother until about 30 weeks of gestation when the foetus begins producing the growth factor on its own. Levels of IGF-1 dramatically decrease in infants born extremely premature (before 28 weeks of gestation), thereby increasing the risk for complications related to the lungs, brain, eyes, and other organs.
A 53% reduction in the incidence of severe BPD
The Phase II top-line data showed a 53% reduction in the incidence of severe BPD, as defined by oxygen challenge testing, in all assessed patients that received SHP607, as compared to untreated infants; and an 89% reduction in those who achieved the prespecified target drug exposure, based on serum concentrations of IGF-1, as compared to untreated infants. The data also showed a 44% reduction in the incidence of severe IVH (Grade III and IV on centrally read ultrasounds) in all assessed patients that received SHP607, as compared to untreated infants; and a 64% reduction in those who achieved the prespecified target drug exposure based on serum concentrations of IGF-1, as compared to untreated infants. The secondary endpoint of time to discharge from neonatal intensive care was not met.
“This is the first controlled clinical trial to confirm the crucial role of IGF-1 in maturation of extremely preterm children,” said Professor Neil Marlow of the University College London Hospitals, UK, and one of the clinical trial investigators. “The reduction in BPD and IVH, as the two most important morbidities suffered by these children, are welcoming and a first in neonatal medicine. It will be important to confirm these findings in additional clinical studies.”
Philip J. Vickers, Ph.D., Head of Research & Development, Shire, said, “Although the study did not meet its primary endpoint, we are extremely encouraged by the topline secondary endpoints related to lung and brain.”