Coeliac UK ‘welcomes’ NICE’s coeliac guidance – but is it too little, too late?
Posted: 14 November 2016 | | No comments yet
Coeliac UK’s Director of Policy, Research & Campaigns, Norma McGough, welcomes NICE’s new quality standards on coeliac disease, which she believes will bring clarity and improvement to diagnosis screening and better access to long term treatment…


On the 19th October 2016, the National Institute of Health and Care Excellence (NICE) published the first quality standard on coeliac disease.[1] This standard is underpinned by the NICE guideline that was published last year and encompasses recognition, assessment and management of coeliac disease.[2]
The new standard sets out five key areas to drive measurable improvements in care of patients with coeliac disease in recognition, diagnosis, support and health for adults and children. This is key as in the context of current rationalisation of resource within the NHS, there is a real risk that management of coeliac disease may become marginalised, as it is a disease that to all intents and purposes is ‘self-managed.’ The Health & Social Care Act 2012 sets out a clear expectation that the care system should consider NICE quality standards in planning and delivering services[3].
“there is a real risk that management of coeliac disease may become marginalised”
With only 24% of the 1 in 100 currently diagnosed in UK we still have a long way to go to raise awareness within healthcare settings, in particular primary care and also with the general public, in order to identify the remaining 500,000 people with the disease.[4]
Benefits of early recognition
The benefits of early recognition are well documented but the presentation of coeliac disease produces notable challenges for healthcare professionals with its changing face and wide range of symptoms.
Dr Geraint Preest shares his tips for GPs diagnosing coeliac disease, highlighting the prevalence of the autoimmune condition. Source: Coeliac UK
Misdiagnosed as Irritable Bowel Syndrome
Despite having NICE guidance providing a framework for recognition of coeliac disease for the last seven years, patients continue to be misdiagnosed with Irritable Bowel Syndrome (IBS), instead of being first tested for coeliac disease.[5]
Clear targets for screening
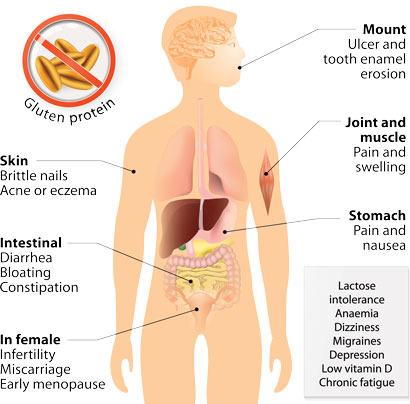

We therefore welcome the new quality standard, providing clear targets, for screening at risk groups of patients, including patients with IBS and for providing a standard timeline for having endoscopy to confirm diagnosis.
Delays in referral for endoscopy after positive serological testing can have a detrimental impact on the outcome of the process. This is because it is essential that patients continue to eat a gluten-containing diet throughout the two-step process for diagnosis.
It may seem simple enough but without this requirement being fulfilled, investigations are a waste of time.
Gluten-free diet as medical treatment
As the gluten-free diet is the medical treatment for coeliac disease it is imperative that gluten is not removed from the diet until a confirmed diagnosis has been made, otherwise the clinical markers used to identify the disease may disappear and the test results may be inaccurate.
If people are symptomatic and the time to endoscopy is prolonged they may be tempted to cut gluten out of their diet to relieve their symptoms. Accurate dietary information is necessary both before, during and after diagnosis of coeliac disease.


Sticking to a gluten free diet is the treatment for Coeliac disease
With reference to dietary management, NICE highlights the importance of referral to a healthcare professional with specialist knowledge of coeliac disease to discuss how to follow a gluten-free diet. The rationale underpinning this recommendation is that it is important for patients with coeliac disease to manage their gluten-free diets, the treatment for coeliac disease, in order to avoid continuing ill health.
High cost of gluten free products
The NICE quality standard also highlights the inequality arising from the higher cost of gluten-free products and the limited availability in small retail outlets. To address this healthcare professionals should help people who may need support find suitable gluten-free foods on prescription.
Annual reviews
The new NICE standard references the importance of offering annual review to patients with coeliac disease and highlights the need for local approaches to encourage as many people as possible to attend with particular reference to socioeconomically deprived areas where people are less likely to attend.
This is an important development as coeliac disease is a treatable disease which requires significant knowledge transfer, lifestyle change and ongoing support to maintain the gluten-free diet treatment and to review patients to screen for preventable long-term complications of the disease.
Check out Coeliac UK’s first ever television advert which hopes to find the half a million people in the UK who are living with coeliac disease without knowing it. Source: Coeliac UK
About the author
Norma McGough began her career as a registered dietitian in the Health Service. In the last 20 years she has worked in the voluntary sector, managing teams at both Diabetes UK and Coeliac UK. Norma currently heads the Policy, Research & Campaigns team and as a member of the senior management team, her role is pivotal in the strategic development of the Charity’s knowledge base.
References
- 1] National Institute of Health & Clinical Excellence (NICE) 2016 quality standard on coeliac disease (QS 134) https://www.nice.org.uk/guidance/QS134
- 2] National Institute of Health & Clinical Excellence (NICE) 2015 recognition, assessment and management of coeliac disease (NG20) https://www.nice.org.uk/guidance/ng20
- 3] http://www.legislation.gov.uk/ukpga/2012/7/pdfs/ukpga_20120007_en.pdf
- 4] West et al 2014 Incidence and prevalence of coeliac disease and dermatitis herpetiformis in the UK over two decades: population based study. Am Journ Gastroenterol 109(5): 757–768
- 5] National Institute of Health & Clinical Excellence (NICE) 2009recognition and assessment of coeliac disease https://www.nice.org.uk/guidance/CG86