Pernicious microorganisms: risks of contamination in pharma
Posted: 18 November 2019 | Julia Fontboté-Duran (Hospital Joan XXIII), Marc Baiget-Francesch (Pharmaceutical Engineer) | 1 comment
Some pharmaceutical manufacturers can struggle to keep microorganisms away from their facilities, which sometimes goes unnoticed until it is too late. While there are numerous threatening microorganisms, this article focuses on some of the most troublesome, highlighting the hazards they pose and analysing how manufacturers can prevent microbial contamination in pharmaceutical plants.
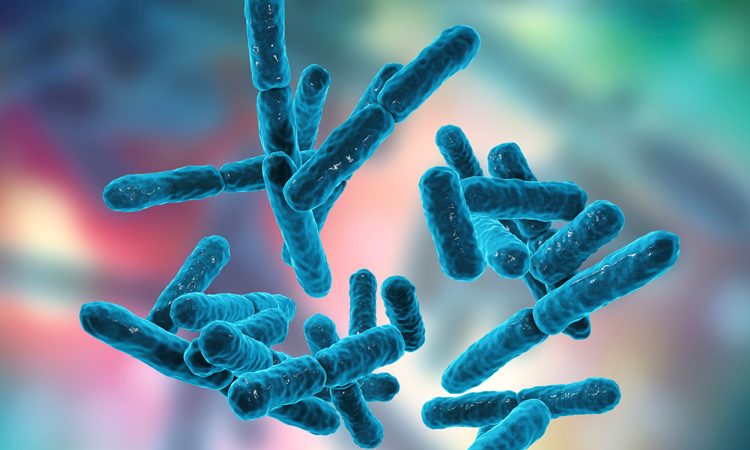

IN MAY 2019, Torrent Pharma Inc. initiated a recall of some of their manufactured pharmaceuticals due to potential microbial contamination.1 The suspected microorganisms, Burkholderia cepacia and Ralstonia pickettii, are well known within the pharmaceutical industry; both microorganisms share certain relevant characteristics, from their ability to proliferate in a broad range of water sources to being especially aggressive against immunocompromised patients. These Gram‑negative bacilli have been linked to Pseudomonas aeruginosa; B. cepacia was formerly known as Pseudomonas cepacia and R. pickettii was first known as Pseudomonas pickettii and then as Burkholderia pickettii before receiving its current name.2,3 These microorganisms typically appear in cystic fibrosis patients and their shared ability to form biofilms is why doctors consider cystic fibrosis a chronic disease.4
Biofilms – an extracellular matrix that confers not only surface adhesion but resistance to external agents and harsh conditions – are one of the main issues that prevents the removal of bacteria in a contaminated system. Eliminating biofilm colonies in humans is almost impossible; this is due to restrictions in the amount of antibacterial agent used. However, attacking the same microorganisms on water pipes of pharmaceutical facilities is, while not easy, more feasible.
On the other hand, if wiping these bacteria from the water systems is easier, why is there still a problem? To begin with, the problem is more complex than it may appear. Firstly, we need to think about detection; how can we attack something that we do not know is there? Classic detection techniques for these organisms are becoming outdated, which makes B. cepacia and R. pickettii harder to identify.5,6 Bacteria culture tests usually take between 24 to 48 hours to return results. Since bacteria like R. pickettii and B. cepacia are known to grow slowly, taking more time than the average microorganism to appear in media plates, false negatives may occur. Furthermore, some problematic bacteria do not grow in the most widely-used culture media.
Eliminating biofilm colonies in humans is almost impossible; this is due to restrictions in the amount of antibacterial agent used”
In the case of B. cepacia, novel media have been described by the USP in a new draft chapter.7 Experts have also pointed out that most of the culture media used for growing such bacteria are rich in nutrients, which does not replicate the environment of microorganisms found in pharmaceutical facilities (where there is a lack of nutrients), potentially leading to false negatives. While new PCR-based detection techniques could help to overcome some of these drawbacks, most pharmaceutical facilities continue to rely on classic techniques.8
Sampling processes are also prone to false negatives. Bacterial biofilms detach and disperse as planktonic cells – biofilm single cells that spread and are more vulnerable to the effects of antibiotics – in irregular patterns. Consequently, sampling may not recreate the reality of the lot subjected to analysis. Further examination will subsequently be continued without the detection of any detachment. In this instance, continuous monitoring, while more expensive, could help to reveal the presence of contaminants faster and more efficiently.
In addition to detection, elimination can also be a problem. Current disinfection routines sometimes do not remove all the bacteria from the pipes; mostly for structural reasons rather than the disinfectant choice. In some cases, the shape of the water pipes enables these bacteria to find shelter in ‘dark spots’, where it is harder for disinfectants to reach, and water filters are generally large enough to allow the passage of these bacteria.9

Product recalls can have a huge impact on a company. Beyond the recall itself, ceasing production, in order to identify the source of contamination that affected the retired batches, can have huge consequences on a company’s financial health, potentially affecting the whole production cycle and schedule. However, it is not just a matter of numbers. B. cepacia and R. pickettii do not present complex clinical cases in most people, but as opportunistic pathogens they are hazardous for immunocompromised patients. For example, in patients with open wounds and catheters, cases of bacteraemia are likely to occur through infected serums and contaminated medical equipment, while cases of endocarditis are common in patients with heart implants. Prosthetic implants’ surfaces can be easily colonised by biofilm-forming communities, making them an ideal infection vector for opportunistic bacteria. For nosocomial infections, a single non-sterile product can be enough to start an outbreak. Furthermore, bacteria in hospitals are under evolutionary pressure, which often results in an enhanced resistance to antibiotics, thus making infections harder to fight.
Ceasing production, in order to identify the source of contamination that affected the retired batches, can have huge consequences on a company’s financial health”
B. cepacia and R. pickettii are presented in this article as the paradigm of resilient, hard-to-detect bacteria that can colonise pharmaceutical facilities. However, there are other similarly problematic bacteria – maybe not at the same level – that cause mayhem within pharmaceutical plants. Gram‑negative bacterial species such as Acinetobacter baumanii, Acinetobacter lwoffi, Flavobacterium aureum, Klebsiella pneumoniae and the already mentioned Pseudomonas aeruginosa, are amongst the most common microorganisms found in pharmaceutical water systems.13 These are all well-known hospital hosts and despite this, continue to cause problems in many medical facilities. Newborns and babies are highly susceptible to infection by these bacteria. Last April, in the Hospital Vall d’Hebron in Barcelona, K. pneumoniae caused the death of two infected babies14 and just a few months later, at least three babies died in a hospital in Pennsylvania because of a Pseudomonas outbreak.15 Although less common, Gram-positive species are sometimes detected in pharmaceutical products. A recent example is a recall issued by Kingston Pharma LLC earlier this year, due to the presence of Bacillus cereus and Bacillus circulans in cough syrup bottles.16
From the examples above, it is evident that the consequences of bacterial contamination in pharmaceutical plants can be serious. To avoid opportunistic bacteria from reaching the hospital, manufacturing facilities should act as the main defence in the fight against bacterial colonisation in pharmaceutical products. Wiping out pernicious microorganisms from pharmaceutical manufacturing facilities would significantly reduce the number of outbreaks. This requires companies to take prevention policies seriously and to implement modern strategies for contamination control. Therefore, spreading awareness of the negative consequences – both economical and human – of failed contamination control can be a huge asset in the fight against opportunistic pathogens.
About the authors




References
- “Urgent: Torrent Pharma, Inc. Issues a Voluntary Recall of …” ASD Healthcare, 6 June 2019, https://www.asdhealthcare.com/AsdHealthcare/media/AsdLibrary/pdfs/News/Torrent-Pharma-Recall-Web-Notice-v2-6-6-19.pdf.
- “Ralstonia Pickettii.” Ralstonia Pickettii – an Overview | ScienceDirect Topics, https://www.sciencedirect.com/topics/medicine-and-dentistry/ralstonia-pickettii.
- “Taxonomy Browser (Burkholderia Cepacia).” National Center for Biotechnology Information, U.S. National Library of Medicine, https://www.ncbi.nlm.nih.gov/Taxonomy/Browser/wwwtax.cgi?mode=info&id=292.
- Lipuma J. “The Changing Microbial Epidemiology in Cystic Fibrosis.” Clinical Microbiology Reviews, American Society for Microbiology (ASM), Apr. 2010, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2863368/.
- Govan JR, et al. “Common Questions About Burkholderia cepacia”
- Ryan, MP, Adley C C. “Ralstonia Spp.: Emerging Global Opportunistic Pathogens. European Journal of Clinical Microbiology & Infectious Diseases. 2013;33(3):291–304
- <60> MICROBIOLOGICAL EXAMINA-TION OF NONSTERILE PRODUCTS—TESTS FOR BURKHOLDERIA CEPACIACOMPLEX.” USP Pharmacopeial Forum, Sept. 2018,
- Lowe C, et al. A Quadruplex Real-Time PCR Assay for the Rapid Detection and Differentiation of the Most Relevant Members of the B. pseudomallei Complex: B. mallei, B. pseudomallei, and B. thailandensis. Plos One. 2016;11
- Gonzalez G, Isabel M, et al. Importancia sanitaria de Pseudomonas aeruginosa en agua de hemodiálisis y su desinfección Revista Cubana De Salud Pública. 2014
- Brooks R B, et al. Multistate Outbreak of Burkholderia Cepacia Complex Bloodstream Infections After Exposure to Contaminated Saline Flush Syringes: United States, 2016– Clinical Infectious Diseases. 2018; 69(3): 445–449
- Chen Y Y, et al. An Outbreak of Ralstonia Pickettii Bloodstream Infection Associated with an Intrinsically Contaminated Normal Saline Solution. Infect Control Hosp Epidemiol. 2017; 38(4) 444–
- Center for Drug Evaluation and Research. “Pfizer Inc. Issues a Voluntary Nationwide Recall for 2 Lots of RELPAX® (Eletriptan Hydrobromide) 40 Mg Tablets Due to Potential Microbiological Contamination of Non-Sterile Products.” S. Food and Drug Administration, FDA, 15 Aug. 2019, https://www.fda.gov/safety/recalls-market-withdrawals-safety-alerts/pfizer-inc-issues-voluntary-nationwide-recall-2-lots-relpaxr-eletriptan-hydrobromide-40-mg-tablets.
- Sandle T. Characterizing the Microbiota of a Pharmaceutical Water System-A Metadata Study. SOJ Microbiology & Infectious Diseases. 2015
- Europa Press. “Cuatro De Los Ocho Bebés Aislados En El Vall D’Hebron Por Klebsiella Mejoran Su Estado De Salud.” es, Europa Press, 30 Apr. 2019, https://www.europapress.es/catalunya/noticia-cuatro-ocho-bebes-aislados-vall-dhebron-klebsiella-mejoran-estado-salud-20190430174953.html.
- Garger K. 3 Infants Die after Bacterial Outbreak at Pennsylvania Hospital. New York Post, New York Post, 8 Oct. 2019, https://nypost.com/2019/10/07/3-infants-die-after-bacterial-outbreak-at-pennsylvania-hospital/.
- Center for Drug Evaluation and Research. “Kingston Pharma, LLC RECALLS ” DG™/Health NATURALS Baby Cough Syrup Mucus’ Because of Possible Health Risk.” S. Food and Drug Administration, FDA, 20 Mar. 2019, https://www.fda.gov/safety/recalls-market-withdrawals-safety-alerts/kingston-pharma-llc-recalls-dgtmhealth-naturals-baby-cough-syrup-mucus-because-possible-health-risk.
Issue
Related topics
Biopharmaceuticals, Bioprocessing, Bioproduction, Drug Manufacturing, Drug Safety, Manufacturing, Microbial Detection, QA/QC
Related organisations
Hospital Vall d’Hebron, Kingston Pharma LLC, Torrent Pharma Inc.








This is interesting information for understanding failed detection methods in pharmaceutical water systems. What are the best strategies to ensure accurate results from microbial testing of water from a pou? Where would you expect to find biofilm in a continuously circulating system?