Maternal immunisation
Posted: 3 March 2016 | | 2 comments
Here, GSK’s Emmanuel Hanon discusses maternal vaccination and how it has emerged as a promising public health strategy…
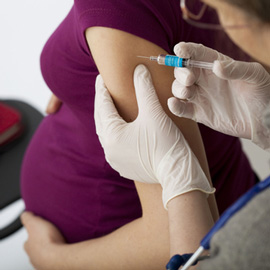

Childhood vaccination was one of the most significant medical success stories of the 20th century with vaccines making diseases such as measles, whooping cough and rubella much more unlikely. New and re-emerging diseases make vaccine discovery a constant challenge as we have recently seen with the Ebola outbreak in West Africa. The field of maternal immunisation is an exciting opportunity supporting the potential development of the vaccines of tomorrow.
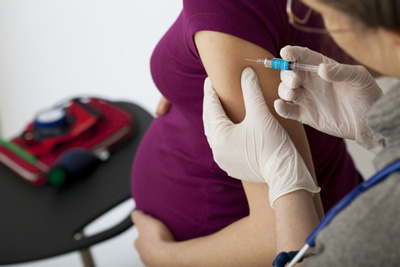

The world has made tremendous strides in reducing child mortality, but there is a still long way to go. Last year UNICEF estimated that almost 6 million children under the age of five will still die every year, equivalent to 11 every minutei. More than a third of these deaths are attributed to infectious diseasesii The fight to reduce global maternal mortality has also progressed, however, recent figures from UNICEFiii report an average of 210 maternal deaths per 100,000 live births, which is still an unacceptably high rate.
In most countries vaccination is first offered to infants at 2 months of age. However, in the past decade, maternal vaccination has emerged as a promising public health strategy, since it has been shown to provide protection against infectious diseases to the mother, her developing foetus and later in newborn infant. There are several examples of successful maternal immunisation strategies such as vaccination against influenza, whooping cough and tetanus.iv In developing countries, the success of maternal tetanus vaccination serves as “proof-of-concept” that maternal immunisation can help protect neonates and infants. In 2013, the WHO reported a 94% reduction in neonatal tetanus compared to the 1980’sv.
GSK is one of the key players in the field of maternal immunisation. An investigational vaccine against Respiratory Syncytial Virus (or RSV), a virus causing acute respiratory infections in nearly 65 million infants and children per year, and killing around 160,000,5 is currently in Phase II trials, and if successful is planned to advance to Phase III by 2019. GSK is also working on an investigational maternal immunisation vaccine for Group B streptococcal infection (GBS), a rarer but deadlier infection compared to RSV. An earlier trivalent version of the GBS vaccine has been tested in clinical trials in 700 women already, and focus has now shifted to the development of a pentavalent type which is potentially expected to offer broader protection against the disease.
As always when introducing a new technology, there are challenges to overcome. One of the challenges in developing a vaccine for maternal immunisation, like GBS, is designing clinical trials in pregnant women that will provide adequate efficacy and safety data.
One option is to use a surrogate endpoint to support vaccine licensure. This is an alternate indicator of effectiveness that can determine efficacy of a vaccine candidate when the burden of disease generally is low or there is no comparator vaccine. One example of how this has been successfully deployed is GSK’s Bexsero vaccine against meningococcal B infection, which was approved for use by the FDA on the basis of immunogenicity endpoints.
There is a global consensus and commitment to exploring the use of maternal vaccination to curb infant mortality. In May 2012, the Global Vaccine Action Plan Vision for universal access to immunisation (GVAP), endorsed by the 194 Member States of the World Health Organisation (WHO) included the use of vaccination during pregnancy. More recently, in 2014, the Global Vaccine and Immunization Research Forum, co-sponsored by WHO and The Bill and Melinda Gates Foundation, presented its maternal immunisation platform targeting influenza, RSV, pertussis, GBS and tetanus.
It is beyond doubt that we are at the beginning of an exciting new era in Vaccinology. A current example that scientists will be considering now is the Zika emergency which may rely on maternal immunisation to help protect infants. What there is consensus on is that, in years to come, maternal immunisation will likely have an increasingly important role to play in improving public health.
References
- http://www.data.unicef.org/child-mortality/under-five.html accessed 10/02/2016
- http://data.unicef.org/maternal-health/maternal-mortality.html accessed 10/02/2016
- http://www.ncbi.nlm.nih.gov/pubmed/23507974 accessed 10/02/2016
- http://www.who.int/immunization/diseases/tetanus/Lancet-2013-Global-child-mortality.pdf?ua=1 accessed 12/02/2016
- http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3255794/ accessed 10/02/2016
Biography
Emmanuel joined Vaccines in 2001 taking roles of increasing responsibility in Immunology and Human Cell mediated immunity before leading the viral vaccines programme in R&D. After heading the Elderly vaccines franchise, playing a critical role in the development of our flu pre-pandemic and pandemic strategy, he was appointed Senior Vice President – Vaccine Discovery and Development in August 2011. Prior to joining GSK, Emmanuel obtained a PhD at University of Liège in the field of Immunology and herpes virology and occupied a post-doctorate position in the field of retrovirology at Imperial College in the UK before moving to Eli Lilly as Associate Scientist in the Toxicology Department. |






I wonder whether there is any recent result that is revealing the effect of mother immunization, done a month or two before the beginning of pregnancy. Maybe such immunisation could still have the positive effects, but would possibly eliminate the negative effects of infectious exposure or maternal immunization during pregnancy associated with epilepsy, or cerebral palsy in children.
Maternal immunisation is currently receiving a lot of attention, and the thinking behind its potential efficacy appears clear. However, given what we are now begining to understand about the neurodevelopmental sequelae of maternal immune activation, and the protean phenotypic manifestations thereof, are we clear that maternal immunisation will not be associated with a very long tail of neurodevelopmental disorders? Please see abstract below:
Nat Rev Neurol. 2014 Nov;10(11):643-60. doi: 10.1038/nrneurol.2014.187. Epub 2014
Oct 14.
Maternal immune activation and abnormal brain development across CNS disorders.
Knuesel I(1), Chicha L(2), Britschgi M(1), Schobel SA(1), Bodmer M(3), Hellings
JA(4), Toovey S(5), Prinssen EP(1).
Author information:
(1)Roche Pharma Research and Early Development, Roche Innovation Centre Basel,
Grenzacherstrasse 124, 4070 Basel, Switzerland. (2)Brain Ischemia &Regeneration
Group, Department of Biomedicine, University Hospital, Hebelstrasse 20, 4031
Basel, Switzerland. (3)Department of Internal Medicine, Emergency Unit,
University Hospital, Petersgraben 2, 4031 Basel, Switzerland. (4)The Nisonger
Centre, Ohio State University, 1581 Dodd Drive, Columbus, OH 43210, USA.
(5)Pegasus Research, Burggartenstrasse 32, 4103 Bottmingen, Switzerland.
Epidemiological studies have shown a clear association between maternal infection
and schizophrenia or autism in the progeny. Animal models have revealed maternal
immune activation (mIA) to be a profound risk factor for neurochemical and
behavioural abnormalities in the offspring. Microglial priming has been proposed
as a major consequence of mIA, and represents a critical link in a causal chain
that leads to the wide spectrum of neuronal dysfunctions and behavioural
phenotypes observed in the juvenile, adult or aged offspring. Such diversity of
phenotypic outcomes in the mIA model are mirrored by recent clinical evidence
suggesting that infectious exposure during pregnancy is also associated with
epilepsy and, to a lesser extent, cerebral palsy in children. Preclinical
research also suggests that mIA might precipitate the development of Alzheimer
and Parkinson diseases. Here, we summarize and critically review the emerging
evidence that mIA is a shared environmental risk factor across CNS disorders that
varies as a function of interactions between genetic and additional environmental
factors. We also review ongoing clinical trials targeting immune pathways
affected by mIA that may play a part in disease manifestation. In addition,
future directions and outstanding questions are discussed, including potential
symptomatic, disease-modifying and preventive treatment strategies.
PMID: 25311587 [PubMed – indexed for MEDLINE]