UK Government issues guidance after allergic reactions to Pfizer COVID-19 vaccine
Posted: 10 December 2020 | Victoria Rees (European Pharmaceutical Review) | No comments yet
Following reports of the Pfizer/BioNTech COVID-19 vaccine causing anaphylaxis, the MHRA has said those prone to allergic reaction should not receive the jab.

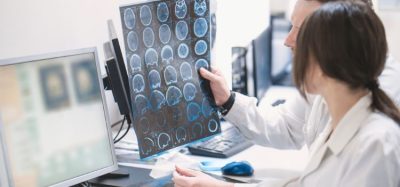
After reports that two UK National Health Service (NHS) workers had allergic reactions to the Pfizer and BioNTech COVID-19 vaccine, the government has released guidance for vaccination centres.
The guidance says that those who are prone to or have a history of anaphylaxis to a vaccine, medicine or food should not receive the Pfizer/BioNTech vaccine. Furthermore, a second dose should not be given to anyone who has experienced anaphylaxis following administration of the first dose of this vaccine.
The guidance also says that vaccine recipients should be monitored for 15 minutes after vaccination, with a longer observation period when indicated after clinical assessment.
Dr June Raine, Chief Executive of the Medicines and Healthcare products Regulatory Agency (MHRA), said: “We have this evening (Wednesday 9 December 2020) issued updated guidance to COVID-19 vaccination centres about the management of anaphylaxis, following two reports of anaphylaxis and one report of a possible allergic reaction following immunisation. This guidance confirms the precautionary advice to healthcare professionals which we issued yesterday evening. Today we convened an Expert Group of the Commission on Human Medicines’ (CHM), attended by experts in Allergy and Clinical Immunology, to robustly review these reports to consider any possible mitigation on the rare risk of anaphylaxis.”
The government has emphasised that anyone due to receive their vaccine should continue with their appointment and discuss any questions or medical history of serious allergies with the healthcare professional prior to getting the jab.
“We have in place a robust and proactive safety monitoring strategy for COVID-19 vaccines which allows for rapid, real-time safety monitoring at population level. The fact that these incidents were picked up and reviewed shows that to be the case. Members of the public and healthcare professionals are encouraged to report suspected side effects through the Yellow Card scheme. We supplement this form of safety monitoring with analysis of data on national vaccine usage and anonymised GP-based electronic healthcare records, linked to other healthcare data, to proactively monitor safety,” said Raine.
Related topics
Drug Safety, Immunisation, QA/QC, Regulation & Legislation, Vaccines
Related organisations
BioNTech, Pfizer, UK Medicines and Healthcare products Regulatory Agency (MHRA)