Could acoziborole eliminate sleeping sickness in Africa?
Acoziborole showed significant success in clinical studies, suggesting it could simplify treatment and help eradicate sleeping sickness.
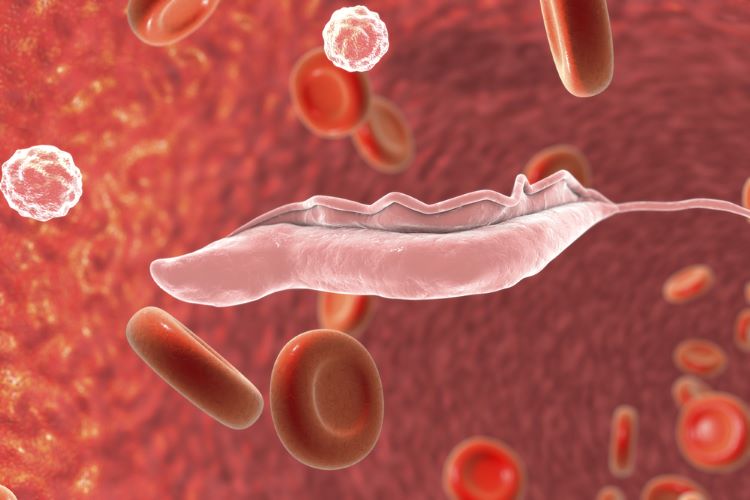
Results from a Phase II/III study, published in The Lancet, showed a single, oral dose of acoziborole was up to 95 percent successful in treating sleeping sickness (human African trypanosomiasis).
About the Phase II/III study
Between 2016 and 2019, DNDi and its partners led an open-label, Phase II/III study to assess the safety and efficacy of acoziborole in patients with early- and late-stage g-HAT. 208 patients were recruited at 10 hospitals in the Democratic Republic of the Congo (DRC) and Guinea.
The 18-month treatment success rate for acoziborole was 95 percent in late-stage g-HAT patients, corresponding to the most positive results from studies with existing treatments (94 percent). In addition, all of the 41 patients with early-stage g-HAT were considered as treatment successes at all timepoints. The study demonstrated acoziborole has a favourable safety profile, with no significant drug-related safety signals reported.
Potential of acoziborole for sleeping sickness
Dr Wilfried Mutombo Kalonji, The Drugs for Neglected Diseases initiative (DNDi) Clinical Project Leader and Medical Manager, and co-author of the paper observed: ”We now have the promise of single-dose, oral treatment that doesn’t need to be taken with food, removes the need for hospitalisation, removes the need for complex or invasive diagnosis or disease staging, and requires minimal training.”
Dr Mariame Camara, principal investigator of the study at the HAT Treatment Centre in Dubreka, Guinea and co-author of The Lancet article concluded, “Acoziborole could potentially become the first treatment that would allow doctors to treat people on the spot, once they receive a positive rapid test in their village.”
In alignment with the World Health Organization (WHO) Neglected Tropical Diseases Roadmap strategy, which aims to eliminate sleeping sickness by 2030. Individuals found to have a positive blood test for g-HAT, could be treated with acoziborole via a simple ‘screen-and-treat’ approach.
The findings will be part of Sanofi’s submission to the European Medicines Agency (EMA). Upon the EMA’s positive opinion and local approval, Sanofi will donate acoziborole to the WHO through its philanthropic organization, Foundation S – The Sanofi Collective.
It is estimated 93 percent of all sleeping sickness cases are the result of the gambiense strain of the human African trypanosomiasis (g-HAT). Transmitted by the bite of an infected tsetse fly, sleeping sickness is fatal without treatment.
“We are now on the cusp of a potential treatment that can be given in one day, in a single dose of three pills – this would be a revolution for doctors and communities,” explained Dr Victor Kande, former Neglected Tropical Diseases Expert Advisor at the Ministry of Health of the DRC, principal investigator of the trial, and lead author of The Lancet article.