Sperm-sorting device may improve IVF success
Posted: 4 January 2018 | Dr Zara Kassam (European Pharmaceutical Review) | 1 comment
Women undergoing IVF may become pregnant with fewer treatment cycles thanks to a device that uses an obstacle course to select the fastest and healthiest sperm…
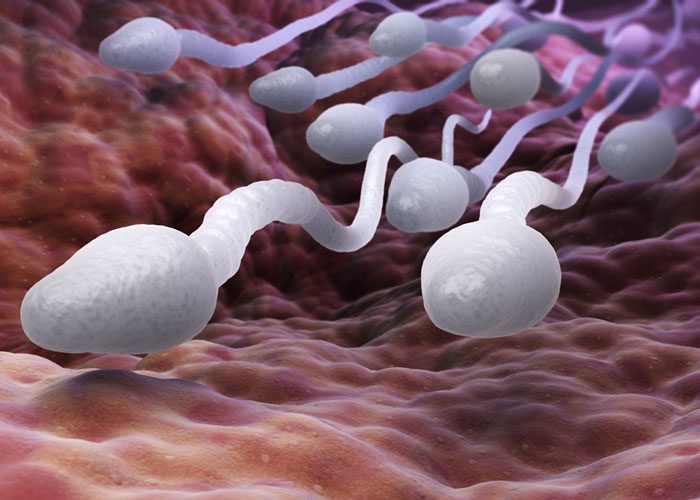

Researchers have developed a new device that uses an “obstacle course” to sort and select faster and healthier sperm cells for in vitro fertilisation (IVF) treatment.
The microfluidic device, which can be used in clinics, is dubbed SPARTAN, short for Simple Periodic ARray for Trapping And IsolatioN. It uses a field of three-dimensional posts that create an obstacle course for the swimming sperm cells. The strongest and healthiest sperm get through this array the fastest and then are collected at the outlet to be used in the IVF process.
Traditional sperm-sorting methods used in IVF treatments select sperm that are the fastest swimmers. The SPARTAN device collects sperm that are the fastest and also the healthiest because it culls out those with malformations, such as bent necks or larger heads, which can slow their movement.
“With SPARTAN, we not only get sperm with excellent motility but also with normal morphology and better DNA integrity, helping families worldwide by reducing the stress of multiple IVF procedures, while potentially increasing pregnancy rates.” said Erkan Tüzel, Associate Professor of physics, biomedical engineering, and computer science at Worcester Polytechnic Institute (WPI). “This could increase patients’ chances of getting pregnant.”
The video depicts the output of a computational model of sperm swimming through a microfluidic sperm sorting device called SPARTAN (Simple Periodic ARray for Trapping And IsolatioN). The device uses a field of three-dimensional posts that create an obstacle course for swimming sperm cells. The layout of the posts assures that the fastest and healthiest sperm reach the output first, which improves the success of the IVF process. Credit: Erkan Tüzel, Worcester Polytechnic Institute (WPI)
The SPARTAN device is about 4 millimetres wide and 12 to 16 millimetres long. Sperm are simply injected into one end and the fastest and healthiest are collected on the opposite end for immediate use in in vitro fertilization. The device also prevents the type of damage to cells that can occur with traditional sorting methods, such as those using high-force centrifuges. Because SPARTAN can be used in the fertility clinic, sperm do not need to be frozen and shipped to a lab for processing; the in-clinic sorting procedure takes between 5 and 30 minutes.
This new sperm-sorting device also could mean that patients will spend less money overall on IVF treatments, which generally cost about $15,000 per cycle because with the new sperm sorting technology they could be able to become pregnant without going through as many treatment cycles.
Prof Tüzel focused his part of the research on modelling the design of the SPARTAN device and used algorithms and fluid physics to model human sperm and how they move in such a complex environment.
Utkan Demirci, Professor of Radiology and electrical engineering at Stanford University, and his team created the overall experimental device designs based on Prof Tüzel’s theoretical models, fabricated and tested the prototypes, and determined the best experimental parameters and medium for the sperm cells to swim through the device.
“Our success was the result of our close collaboration, bringing theory and experiment together–WPI working with the Demirci Lab,” said Prof Tüzel. “And as a physicist, this is very exciting. We’re going to have a product in the market helping people. That doesn’t always happen in physics in such a short time frame, especially if you are a theoretical physicist.”
Prof Demirci said the collaborative work enabled the research teams to create a new technology that can have a real impact at the clinic, potentially leading all the way to live births.
“The collaboration between Erkan’s lab and my lab is invaluable,” he added. “WPI brings an outstanding theoretical tool that allows us to understand how microscale objects, such as sperm, interact with their environment; and we are able to design this know-how into real microfluidic devices, clinically validate what we designed, and experimentally improve it into a real-world application.”
The research has been published in Advanced Science.
Related topics
DNA, Process Analytical Technologies (PAT), Research & Development (R&D)
Related organisations
National Science Foundation, Stanford University, Worcester Polytechnic Institute









Hi,
Wow, a Very Nice blog post! Your site has given the best information From Your Articles. They are amazing and Useful to all people. Thank you for sharing this post and Impressive site. The IVF advanced is one of the most excellent centers in Asia Pacific, with Techniques, genuine Treatment, Research & Training. The IVF advanced is the leading Test Tube Centre in the country with modern world-class scientific technologies.