Stem cells to grow new immune system in Crohn’s disease patients
Posted: 8 August 2018 | Iqra Farooq (European Pharmaceutical Review) | 2 comments
A phase III clinical trial looks to use a patients own stem cells to treat the debilitating disease…
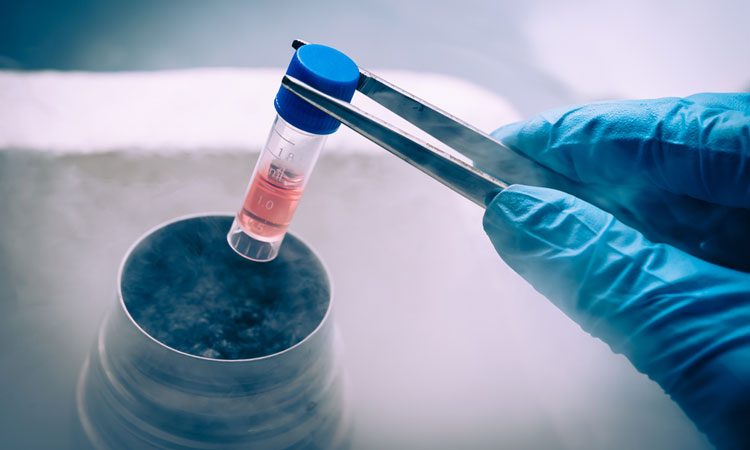

A clinical trial has begun which uses stem cell transplants in patients in order to ‘grow’ a new immune system for people with Crohn’s disease. The trial is led by Queen Mary University, London, and is funded with a £2 million grant from a partnership between the Medical Research Council (MRC) and the National Institute for Health Research (NIHR).
The clinical trial, named ASTIClite, will recruit patients from London, Liverpool, Sheffield, Cambridge, Edinburgh, Nottingham and Oxford and will be coordinated through the Clinical Trials Unit at the University of Sheffield.
Crohn’s disease is a debilitating, chronic, painful intestinal disease affecting over 115,000 people in the UK. It causes inflammation of the lining of the digestive system, resulting in diarrhoea, extreme tiredness, abdominal pain and symptoms which considerably affect the quality of life of patients.
Current treatments aim to reduce the inflammation, with many patients having to undergo surgery to remove the affected areas. Extreme cases involve an operation diverting the bowel to a pouch in the stomach, where stools can be collected.
Recently, stem cells have been successfully used to replace the immune system in patients with multiple sclerosis, and this new clinical trial will investigate whether a similar treatment can reduce gut inflammation, offering hope to patients with Crohn’s disease.
Professor James Lindsay, Chief Investigator, and a consultant at Barts Health NHS Trust said, “Despite the introduction of new drugs, there are still many patients who don’t respond, or gradually lose response, to all available treatments. Although surgery with the formation of a stoma may be an option that allows patients to return to normal daily activities, it is not suitable in some and others may not want to consider this approach.
“We’re hoping that by completely resetting the patient’s immune system through a stem cell transplant, we might be able to radically alter the course of the disease. While it may not be a cure, it may allow some patients to finally respond to drugs which previously did not work.”
During the trial, patients will undergo hormone treatment and chemotherapy to mobilise their stem cells. The cells are then harvested from their blood, and further chemotherapy will be used to ‘wipe out’ their immune system. The stem cells will then be reintroduced to the body, with the aim that they will develop into new immune cells, providing the patient with a working immune system.
Theoretically, a new immune system will no longer act adversely to the patient’s own gut causing inflammation, and will allow drugs administered time to work.
Director of the NIHR Evaluation, Trials and Studies programmes, Professor Tom Walley said, “Stem cell therapies are an important, active and growing area of research with great potential. There are early findings showing a role for stem cells in replacing damaged tissue. In Crohn’s disease this approach could offer real benefits for the clinical care and long term health of patients.”
The clinical trial will involve academics from the University of Nottingham, University of Manchester, University of Oxford, Nottingham Trent University, University of Edinburgh, University of Sheffield, King’s College London, and Queen Mary University of London.
Since this clinical trial is a follow up from a trial that ran in 2015, the researchers can apply results to this study. Some drugs administered initially had serious side effects, and so this time, the researchers look to decrease the dosage of the treatment, minimising toxicity.
More information about the Phase III clinical trial can be found here.
Related topics
Clinical Development, Clinical Trials, Drug Development, Research & Development (R&D), Stem Cells
Related organisations
Clinical Trials Unit University of Sheffield, Medical Research Council (MRC), National Institute for Health Research, Queen Mary University London








Thank God for the brilliant researchers in England who are devoting their energies into finding an alternative method to treating this disease for which my son has suffered with for the past 12 years. He is 27 now and was an outstanding soccer player in the US before this derailed his playing days. Please please continue to work toward rebuilding the immune system defects that cause this horrible debilitating disease.
It’s fascinating that stem cell treatments can help patients with Crohn’s disease to grow new immune systems. My brother was recently diagnosed with Crohn’s disease, and he’s looking into his treatment options. I’ll pass this information along to him so that he can look further into his options for getting stem cell treatments to help with that in the future.