Implantable technology could enable in vivo CAR T therapy
Posted: 31 March 2022 | Hannah Balfour (European Pharmaceutical Review) | No comments yet
Pre-clinical research demonstrates the potential of a new implantable biotechnology called MASTER to produce and release CAR T cells in vivo.

An implantable biotechnology that releases chimeric antigen receptor (CAR) T cells could increase the speed and efficacy of cancer therapy, according to researchers. A pre-clinical proof-of-concept paper evaluating Multifunctional Alginate Scaffolds for T cell Engineering and Release (MASTER) in mice with lymphomas was published in Nature Biotechnology.
CAR T-cell therapies are a type of immunotherapy in which T cells are genetically modified with a CAR gene to express a receptor that causes them to target and destroy cancer cells. These treatments have shown promise in the treatment of haematological cancers, including lymphomas; however, patient access to these treatments is limited because they are highly expensive, costing hundreds of thousands of dollars per dose. One reason for this cost is the complexity and length of manufacturing the treatment.
Autologous CAR T-cell therapies are produced by extracting a patient’s blood, isolating their T cells and sending them to a manufacturing facility where, ex vivo, the cells are activated, genetically modified to express a CAR gene and then proliferated to expand their number. Once the manipulations are complete the reprogrammed cells are brought back to the hospital and infused into patients.
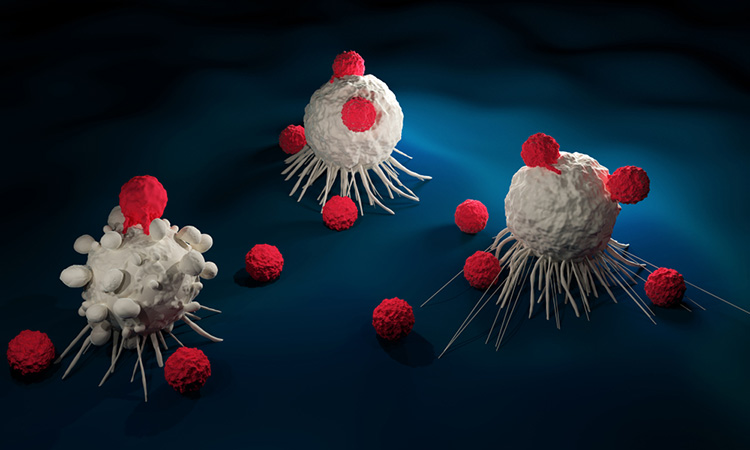
![A bioinstructive scaffold (white) developed by the researchers, produces and releases genetically reprogrammed T cells that target and destroy a growing tumour [Credit: Ella Maru Studio].](https://www.europeanpharmaceuticalreview.com/wp-content/uploads/Multifunctional-Alginate-Scaffolds-for-T-cell-Engineering-and-Release-MASTER-375x211.jpg)
![A bioinstructive scaffold (white) developed by the researchers, produces and releases genetically reprogrammed T cells that target and destroy a growing tumour [Credit: Ella Maru Studio].](https://www.europeanpharmaceuticalreview.com/wp-content/uploads/Multifunctional-Alginate-Scaffolds-for-T-cell-Engineering-and-Release-MASTER-375x211.jpg)
A bioinstructive scaffold (white) developed by the researchers, produces and releases genetically reprogrammed T cells that target and destroy a growing tumour [Credit: Ella Maru Studio].
“Our MASTER technology takes the cumbersome and time-consuming activation, reprogramming and expansion steps and performs them inside the patient,” stated Pritha Agarwalla, lead author of the study and a postdoctoral researcher in the joint biomedical engineering department at North Carolina State University (NC State) and the University of North Carolina at Chapel Hill (UNC). “This transforms the multi-week process into a single-day procedure.”
MASTER is a biocompatible, sponge-like material with the look and feel of a mini marshmallow. To begin treatment, researchers isolate T cells from the patient and mix these naïve (or non-activated) T cells with the engineered virus. This mixture is then poured on top of the MASTER, which absorbs it. MASTER is decorated with antibodies that activate the T cells, so the cell activation process begins almost immediately. Meanwhile, MASTER is surgically implanted into the patient, which, in the current studies, is a mouse.
After implantation, the cellular activation process continues. As the T cells become activated, they begin responding to modified viruses that reprogramme them into CAR-T cells.
“The large pores and sponge-like nature of the MASTER material brings the virus and cells close together, which facilitates cellular genetic reprogramming,” stated Agarwalla.
The MASTER material is also impregnated with factors called interleukins that foster cell proliferation. After implantation, these interleukins begin to leach out, promoting rapid proliferation of the CAR T cells.
To test MASTER, the researchers used mice with lymphoma, treating one with the new implant and the other intravenous CAR T cell therapy. These two groups were compared to control group receiving non-engineered T cells.
“Our technology performed very well,” stated Yevgeny Brudno, corresponding author of the study and assistant professor in the joint biomedical engineering department at NC State and UNC. “It would take at least two weeks to create CAR T cells from naïve T cells for clinical use. We were able to introduce the MASTER into a mouse within hours of isolating naïve T cells.”
In addition, since cells are implanted within hours of isolation, the minimal manipulation creates healthier cells that exhibit fewer markers associated with poor anti-cancer performance in CAR-T cells. Specifically, the MASTER technique results in cells that are less differentiated, said the team, which translates to better sustainability in the body and more anti-cancer potency. In addition, the cells display fewer markers of T-cell exhaustion, which is defined by poor T cell function.
“The end result is that the mice that received CAR-T cell treatment via MASTER were far better at fighting off tumours than mice that received conventional CAR-T cell treatment,” Agarwalla added. The improvement in anti-cancer efficacy was especially pronounced over the long term, when mice were faced with a recurrence of lymphoma.
“The MASTER technology was very promising in liquid tumours, such as lymphomas, but we are especially eager to see how MASTER performs against solid tumours – including pancreatic cancer and brain tumours,” Brudno stated. “We are working with an industry partner to commercialise the technology, but there is still a lot of work to be done before it becomes clinically available. Further work to establish the safety and robustness of this technology in animal models will be necessary before we can begin exploring clinical trials involving human patients.”
While it is impossible to estimate what the cost of MASTER treatment might be if it is eventually approved for clinical use, Brudno stated that he is optimistic that it would be substantially less expensive than existing CAR-T treatment options.
“We are also exploring opportunities with other industry partners for taking the fundamental concepts of MASTER and applying them for use in regenerative medicine and in treating autoimmune disease,” Brudno stated. Agarwalla added: “I feel like we are just scratching the surface of what is possible here.”
The work was done with support from the North Carolina Biotechnology Center, under flash grant 2019-FLG-3812; from the National Center for Advancing Translational Sciences; and from the National Institutes of Health under grants UL1TR002489, R01CA193140, R21-CA229938-01A1, T32CA196589 and R25NS094093.
Related topics
Anti-Cancer Therapeutics, Biologics, Biopharmaceuticals, Bioproduction, Drug Delivery Systems, Drug Development, Immunotherapy, Medical Devices, Preclinical Research, Research & Development (R&D), t-cells, Technology
Related organisations
North Carolina State University, University of North Carolina at Chapel Hill