Stroke imaging technology could reduce potential for brain damage
Posted: 2 August 2018 | European Pharmaceutical Review | No comments yet
The researchers suggest that stroke patients may be able to avoid CT scans or the emergency department, and go directly the angiosuite…
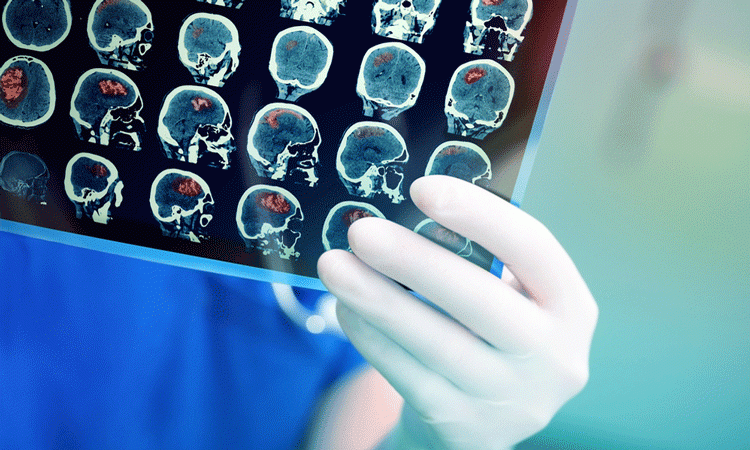

A current study has found that new stroke imaging technology could decrease delays in care by up to 60 minutes, giving a better chance of a full recovery to patients.
The study was called ‘New Multiple CT Assessment of Acute Stroke Patients: Are We Ready Prime Time?’ and shows that recent advances in imaging software in the angiosuite gives neurointerventionalists the vital details that are essential in diagnosing patients with large vessel occlusion (LVO) for an endovascular thrombectomy. LVO is the acute blockage of a proximal vessel, such as the middle of the cerebral artery, and often leads to ischemic strokes.
Lead author of the study and an interventional clinical research technologist at Toronto Western Hospital, Nicole Cancelliere said, “by using this technology in the angiosuite, hospitals can reduce intra-facility transfer delays and hence the time of stroke symptom onset to treatment, which will significantly reduce brain damage and improve outcomes for patients.”
The time required to transfer a patient from their CT scan to the operating table could delay the endovascular thrombectomy by as long as one hour.
The preliminary results of the study show that the cone beam imaging software compares favourably with baseline and follow up CT scans. This imaging technique allows more accurate detection of haemorrhage, the occlusion site, other tissue at risk and the ischemic core. The team propose that cone beam imaging software can be used as baseline imaging.
The principle investigator on the study, Professor Vitor Mendes Pereira concluded, “By reducing intra-facility transfer times, patients can receive endovascular thrombectomy treatment sooner, which can significantly impact patient outcomes.”
The researchers suggest that in the future, stroke patients may be able to avoid CT scans or the emergency department and go directly the angiosuite for proper care and advanced imaging.
The study was presented at the 15th annual meeting of the Society of Neuro-Interventional Surgery’s (SNIS).
Related topics
Analytical techniques, Clinical Development, Research & Development (R&D)