Advancing cell therapies – γδ T cells and the combination factor
Posted: 13 July 2022 | Hannah Balfour (European Pharmaceutical Review) | No comments yet
In this Q&A, Bryan Kobel, Chief Executive Officer of TC Biopharm, discusses innovations in cell therapies, introducing the company’s work in gamma delta (γδ) T-cell technologies and his predictions for the future of cell therapy development.

Please give some background on TC BioPharm and its aims
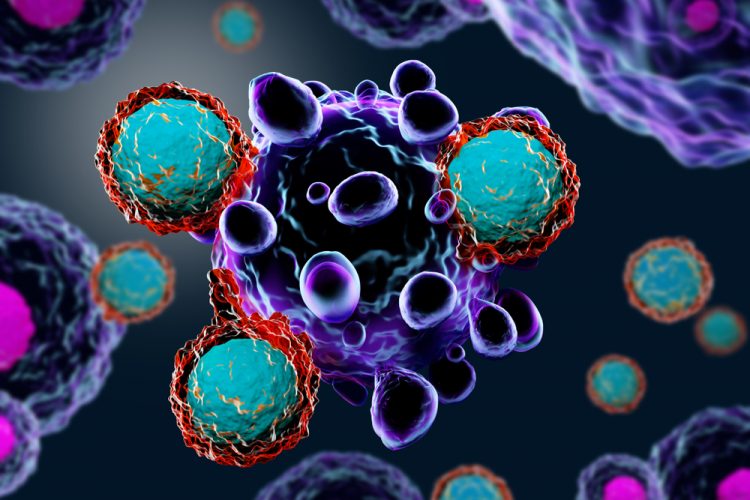
Kobel: As the global leader in allogeneic gamma delta (γδ) T-cell technologies, we are focused on the use of our platform allogeneic γδ T cells from healthy donors as a therapeutic for oncology indications. Right now, we are targeting blood cancers, with clinical data in relapsed/refractory acute myeloid leukaemia (AML), and moving into solid tumours, most likely in some version of a combination therapy or as a modified γδ such as a chimeric antigen receptor (CAR).
Our work is establishing whether it is possible to use allogeneic innate immune cells from a healthy donor to support the immune system of a person with cancer in combatting the condition. It is really the idea of reinforcing nature and letting the immune system do what it was intended to do, which is use this universal, inherent killer to fight diseases.
Why gamma delta T cells?
Kobel: There is no bad cell therapy out there, but all therapies have limitations – there is no such thing as a limitless cell therapy or drug. CAR T-cell therapies, for example, have two: firstly, because they are typically autologous (ie, use a patient’s own cells), some patients are simply too sick to be able to donate cells to produce the treatment.
Additionally, CARs target T-cell receptors, and those receptors happen to exist on both healthy and diseased cells, so they can destroy both, causing what is called “onsite off tumour toxicity”. This toxicity limits the possible dose that can be given to patients, so it is hard to give a sufficiently large dose to enable the treatment to leave the vasculature and permeate tissues to interact with and fight solid tumours.
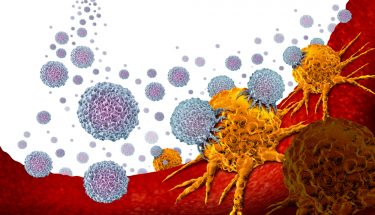

γδ T cells are the first line of defence in the immune system to eradicate diseases. They have an inherent ability to seek out and destroy damaged and diseased cells due to the presence of an antigen called isopentenyl pyrophosphate, or IPP for short. All tumours ever discovered and studied emit IPP, while healthy cells do not.
γδ T cells act somewhat like a shark smelling blood; when they sense IPP, the cells slowly make their way towards the concentration until they find the source and affect cell death.
What is beneficial about them is that they have a limited toxicity profile; they have very few side effects, unlike traditional cancer treatments such as chemotherapy. You can also give them to people in conjunction with other drugs because there is no drug-on-drug profile.
Gamma delta T-cell biology
γδ T cells are ‘unconventional’ T cells and there are relatively few present in peripheral blood. Unlike their better know CD4+ helper T cell and CD8+ cytotoxic T cell cousins, which express alpha beta (αβ) T-cell receptors (TCRs), they express TCRs composed of γ and δ chains.
In contrast to αβ T cells, the majority of γδ T cells are activated in a major histocompatibility complex (MHC)-independent manner, by both self and non-self ligands. Self ligands that activate γδ T cells in a TCR-dependent manner include IPP, often accumulated by cancer cells, and other markers of cellular stress resulting from infection or tumorigenesis. In response, γδ T cells produce cytokines, chemokines, interact with other immune cells and affect cytolysis of infected or transformed target cells.
As tissue-associated populations of γδ T cells have been identified in the epithelium and mucosa, scientists believe they may serve as the first line of defence against pathogens.
Source: Eberl M, Hayday A. Gamma Delta (γδ) T Cells, British Society for Immunology.
For what indications are gamma delta T cells being developed?
Kobel: We are currently in a Phase IIb/III clinical trial for AML using γδ T cells as a second-line therapy, also known as a failed first-line induction. This is a bridge to bone marrow or stem-cell transplant, which is the next step in your standard of care.
The data from our Phase Ib/IIa trial in AML was positive, so we are excited to see if we can replicate these results in other blood cancers, acute lymphoblastic leukaemia (ALL), chronic lymphocytic leukaemia (CLL) and multiple myeloma, through some form of an umbrella trial.
I think the way forward for cell therapy is in combining therapies; so not developing monotherapies but instead combining the benefits of two or more treatments, for instance, γδ T cells and checkpoint inhibitors or natural killer (NK) cells”
In the Phase Ib/IIa study, the average blast count (measured disease) in patients when they entered the trial was 38 percent; 28 days later, after one dose of γδ T cells, their average blast count had been reduced to six percent, which is borderline remission.
We saw two complete responses including one MLFS or morphological leukaemia-free state, which means they were no longer leukemic. One patient went from a 60 percent blast count to 10 percent within 28 days and another patient lived more than two years after the trial.
These results were really encouraging, especially in patients that were in palliative care – expected to live four to six weeks. We are excited to see what these therapeutics can do in healthier patients, which conceptually should have a better response.
We are also starting to look at solid tumour opportunities in combination with other partners; investigating prostate, pancreatic, colorectal, ovarian and head and neck cancers.
We have developed a costimulatory CAR approach specifically for solid tumours such as ovarian cancer, neuroblastoma and glioblastoma, which is designed to overcome off-tumour toxicity. This is achieved by taking the CAR T-cell receptor and combining it with the γδ T cells’ function around IPP. The therapeutic cell expresses both CAR and γδ receptors.
Say the expressed CAR receptor is for CD19; if the CAR binds to a cell expressing CD19 but not IPP, then the γδ receptor does not bind and the therapeutic cell detaches. However, if the cell expresses both CD19 and IPP, and therefore both the CAR and γδ receptors bind, then it completes a biological circuit that kills the cancerous cell. Because of this on-off switch, the damage to healthy cells is minimised and we should therefore be able to dose patients with larger amounts of these CAR γδ T cells safely, allowing them to escape the vasculature and enter tissues to reach tumours in the organs.
How do you envision cell therapies developing in future?
Kobel: Development in the cell therapy landscape is akin to how Ernest Hemingway described going broke; it happens very slowly at first then all of a sudden. Right now, technology is advancing so quickly it is incredible.
Personally, I think the way forward for cell therapy is in combining therapies; so not developing monotherapies but instead combining the benefits of two or more treatments, for instance, γδ T cells and checkpoint inhibitors or natural killer (NK) cells. We believe γδ T cells can form the backbone of these combinations going forwards, given their innate ability within the immune system and their function as tumour killers.
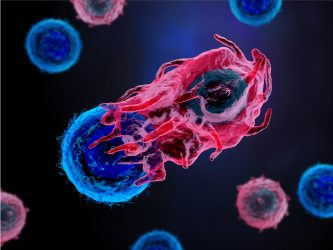

We are very excited by the progress being made in the NK cell arena, as combining allogeneic NK cell infusions with γδ T-cell infusions could be an interesting dynamic. We are of the mindset that you can rebuild, or recreate, the immune system to a certain degree artificially.
Conceptually, you could receive an infusion of γδ T cells, then repeated infusions of NK cells for several weeks before a further γδ T-cell infusion. Repeating this over and over, to the extent that you are basically taking an exogenous version of the immune system, could provide efficacy with limited toxicity.
We also think combining cell therapies with checkpoint inhibitors and bispecific antibodies is interesting, as it could help overcome the iceberg problem. Existing treatments such as checkpoint inhibitors can be limited to accessing the tip of the iceberg when it comes to cancers; they benefit patients with a stable immune system that is able to proliferate immune cells such as γδ T or NK cells. But if you do not have a stable immune system, ie, it is suppressed or compromised, which is the case for the majority of patients, it does not matter how many times you try to invigorate an immune response – the immune system is unable to respond. We are excited to see how combining checkpoint inhibitors and the exogenous infusion of immune cell therapies could benefit patients.
Which challenges must be overcome to continue to advance cell therapies?
Kobel: There is a major bottleneck across all cell therapies and that is supply and demand for the base product of cells. Companies are continually building manufacturing plants to support production, as well as advancing allogeneic technologies to remove certain burdens, both of which are great. However, if we really want to use cell therapies in the way that I believe they can be used, which is not just in oncology but in numerous areas including viral and inflammatory diseases, etc, there are not enough donors to support the potentially vast needs of product creation.
The next step is really developing what we call a “universal donor”, which would be induced pluripotent stem cell (iPSC) lines that can produce the requisite cell types, whether they be γδ T cells, NK cells, macrophages or αβ T cells.
We must solve this supply-demand bottleneck, so over the next five to 10 years, I anticipate the removal of the donor entirely and the use of iPSCs as the source for production instead.
Bryan Kobel is the Chief Executive Officer of TC Biopharm and joined the company in June 2021. Bryan has been active in healthcare and life sciences for over 15 years, advising private and public companies on capital structuring and sourcing, and bringing a broad range of investors from private family capital to traditional corporate venture investors to his clients.
About TC Biopharm
TC BioPharm is a publicly-traded (TCBP), clinical-stage cell therapy company developing advanced allogeneic CAR T-cell therapy products for the treatment of cancer, as well as developing gamma delta T-cell therapies for the treatment of infectious disease. The company was established in 2014 and now has five global locations, with its headquarters in Glasgow, Scotland, UK.
About the author
Hannah Balfour is the Science Writer for European Pharmaceutical Review
Related topics
Biologics, Bioproduction, Clinical Development, Clinical Trials, Drug Development, Drug Safety, Drug Targets, Personalised medicine, Research & Development (R&D), t-cells, Technology, Therapeutics









