Ultrasound delivers antibody therapy for HER2-positive brain metastasis
Posted: 14 October 2021 | Anna Begley (European Pharmaceutical Review) | No comments yet
MR-guided focused ultrasound safely delivered antibody therapy to breast cancer that has metastasised to the brain in Phase I study.

Researchers at the Sunnybrook Health Sciences Centre, Canada, have demonstrated that magnetic resonance (MR)-guided focused ultrasound can be used to safely deliver antibody therapy to breast cancer that has metastasised to the brain.
In this Phase I clinical trial for HER2-positive breast cancer patients, published in Science Translational Medicine, the Sunnybrook team captured images of the monoclonal antibody therapy, trastuzumab, precisely targeting tumours in the brain after using Insightec’s Exablate Neuro focused ultrasound device to temporarily and non-invasively open the blood-brain barrier (BBB) and enable intravenous trastuzumab to more effectively access tumour sites of four patients.
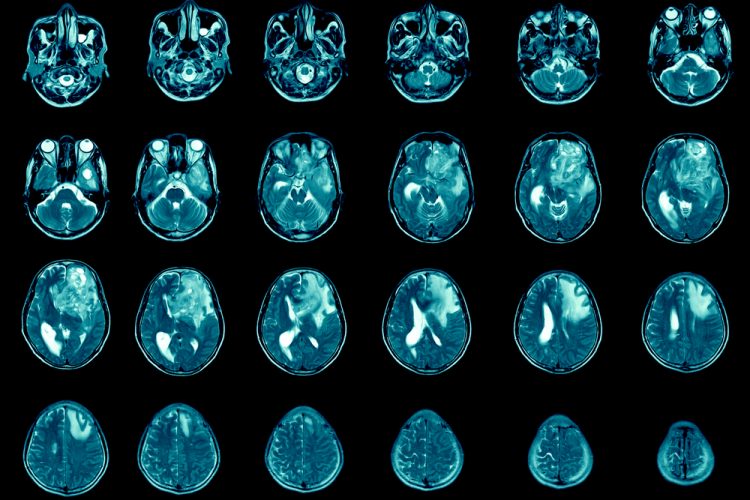
![MR images showing reduction in size of metastatic tumors after focused-ultrasound delivery of antibody therapy through blood-brain barrier [Credit: Sunnybrook Health Sciences Centre].](https://www.europeanpharmaceuticalreview.com/wp-content/uploads/MR-focused-ultrasound-brain-metastases.png)
![MR images showing reduction in size of metastatic tumors after focused-ultrasound delivery of antibody therapy through blood-brain barrier [Credit: Sunnybrook Health Sciences Centre].](https://www.europeanpharmaceuticalreview.com/wp-content/uploads/MR-focused-ultrasound-brain-metastases.png)
MR images showing reduction in size of metastatic tumors after focused-ultrasound delivery of antibody therapy through blood-brain barrier [Credit: Sunnybrook Health Sciences Centre].
This first-in-human trial suggests that MR-guided focused ultrasound is a safe and effective method to deliver treatments across the BBB and paves the way for the use of this method for other neurological conditions. “This is the first visual confirmation that focused ultrasound can improve the delivery of targeted antibody therapy across the BBB,” explained Dr Nir Lipsman, the study’s principal investigator. “These are preliminary, but very promising, results that with continued research have implications well beyond brain cancer for other neurological conditions, including Parkinson’s disease and Alzheimer’s, where the blood-brain barrier poses a challenge to drug delivery.”
These results set the stage for the possibility of delivering a host of both established and novel therapies for numerous brain conditions that otherwise cannot gain access to the brain. “The early data in this study suggests delivery of antibody therapy directly to tumours using focused ultrasound may impact treatment efficacy, with tumours slightly decreasing in size, with varying results for patients between seven and 31 percent during the study – on average to 21 percent,” added oncologist Dr Rossanna Pezo. “The reduction in tumour size is promising but should be interpreted with caution as further research on a larger scale is needed.”
Related topics
Anti-Cancer Therapeutics, Antibodies, Clinical Trials, Drug Delivery Systems, Research & Development (R&D), Therapeutics, Ultrasound