Rivaroxaban reduced blood clots and related death in cancer patients
Posted: 4 December 2018 | European Pharmaceutical Review | No comments yet
Through a clinical trial, Cleveland researchers have identified how rivaroxaban reduces blood clots in cancer patients and also decreases related deaths…
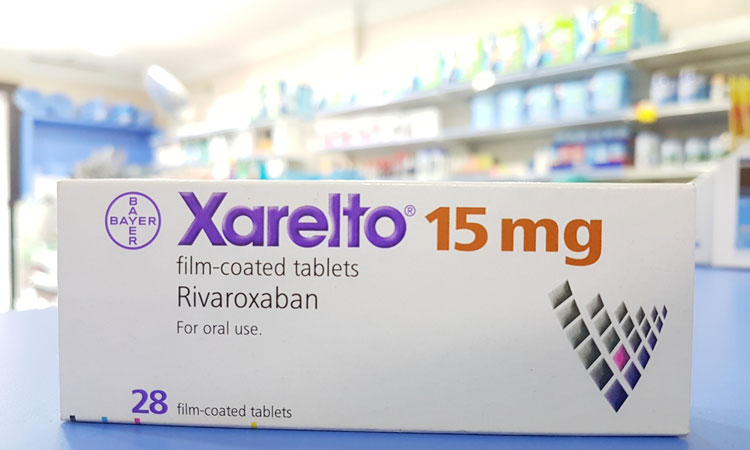

A study has found that rivaroxaban reduces venous thromboembolism related deaths in patients.
Cleveland Clinic medical oncologist and researcher, Dr Alok Khorana, is the primary investigator on a study that concluded rivaroxaban for venous thromboembolism (VTE), a blood clot in the venous system, significantly reduced VTE and VTE-related death for outpatient, at-risk cancer patients while they were taking the oral blood thinner.
During the on-treatment period, blood clots occurred less frequently (2.62 percent) in patients taking rivaroxaban, compared to and 6.41 percent of the placebo groups. However, during the full study period – which included 180-day observation after the medication was stopped – the gap narrowed with blood clots occurring in 5.95 percent of patients in the rivaroxaban group, compared to 8.79 percent of the placebo groups.
Those taking rivaroxaban were less likely to die – 23.1 percent, compared to 29.5 percent in the placebo group for the combined endpoint of all-cause death and VTE. Major bleeding, a dangerous side effect of anticoagulants, occurred in less than 2 percent of patients – on par with what would be expected with prophylactic anticoagulation in cancer patients.
“These results tell us that rivaroxaban effectively prevents blood clots in at-risk cancer patients during the treatment period,” said Dr Khorana. “Post-treatment, risk of VTE persists, with one-third of VTE or VTE-related death occurring in patients after rivaroxaban was discontinued.”
This is the first time extended outpatient interventions to prevent blood clots in an at-risk cancer patient population has been tested with direct oral anticoagulants. Results were presented at the American Society of Haematology (ASH) Annual Meeting.
Blood clots are the second leading cause of death for cancer patients after cancer itself. One in five cancer patients will get a blood clot at some point during the natural history of their illness.
“Cancer patients can have complications – such as blood clots – from cancer itself, or from cancer treatment,” said Dr Khorana. “These complications are distressing for patients, may delay treatment, and contribute to emergency room visits and hospitalisations which impact healthcare utilisation and costs.”
Often cancer patients are administered blood thinners to prevent blood clots in the hospital setting, however, because cancer treatment is typically an outpatient procedure, most cancer-related blood clots occur out of the hospital. Current options for outpatients at risk for blood clots, studied by previous clinical trials, are low-molecular-weight heparins, which are injections that the patient must administer daily.
A patient’s risk of blood clots was identified at the time of chemotherapy initiation by the Khorana Score, designed by Dr Khorana. The score predicts blood clots based on a collection of simple variables – type of cancer, body mass index and complete blood count (platelet, leukocyte, hemoglobin). Cancer patients with a Khorana score of 2 or greater are considered at higher risk for developing blood clots, and were included in the trial.
The primary endpoint in the double-blind, randomised, placebo-controlled, parallel-group, multicenter study was VTE or VTE-related death. Patients were randomised 1:1 to rivaroxaban 10 milligrams once daily or placebo for 180 days, and were checked for clots at the onset of the trial.
“This signals a change in the prevention approaches to cancer-associated VTE,” said Dr Khorana. “We are moving into a new era of direct oral anticoagulants.”
Study results should inform future recommendations regarding the prevention of blood clots in at-risk ambulatory cancer patients.
Related topics
Analytical techniques, Clinical Development, Clinical Trials, Drug Development, Research & Development (R&D)