Trial of new HIV PrEP medication stopped early due to effectiveness
Posted: 10 November 2020 | Hannah Balfour (European Pharmaceutical Review) | No comments yet
The trial was stopped because the data suggested that injections of the long-acting antiretroviral drug cabotegravir (CAB LA) are highly effective for HIV pre-exposure prophylaxis (PrEP) in women.
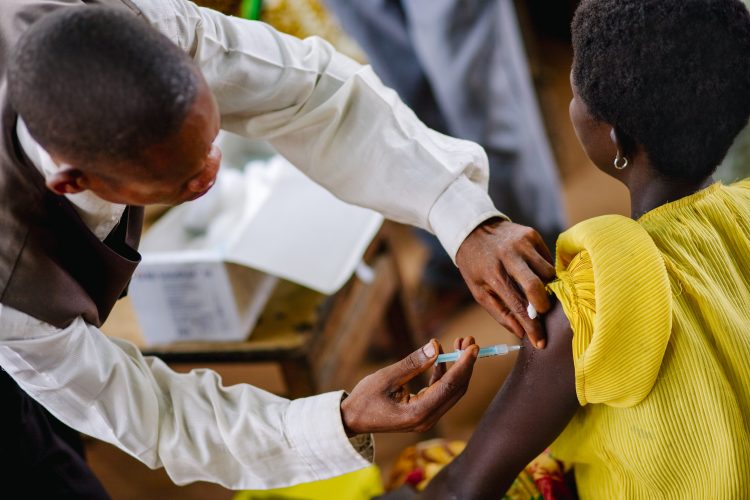

The HIV Prevention Trials Network study (HPTN 084) evaluating the long-acting injectable antiretroviral drug cabotegravir (CAB LA), for pre-exposure prophylaxis (PrEP) in HIV-uninfected women, has been stopped early by the trial Data and Safety Monitoring Board (DSMB) as results showed CAB LA to be highly effective in preventing HIV acquisition.
Women in sub-Saharan Africa continue to experience high HIV incidence. While oral PrEP is highly effective in preventing HIV in women when taken as prescribed, difficulties with patient adherence reduce its protective effect. Therefore, more effective and acceptable HIV prevention choices for women are needed. A long-acting injectable formulation has the potential to improve the prevention effect without relying on adherence to a daily oral PrEP regimen.
HPTN 084 trial design
In total, 3,223 sub-Saharan African women between the ages of 18 and 45 were enrolled in the trial. The participants from 20 sites across seven countries were randomised into two arms:
- Arm A – CAB LA (as an intramuscular injection every 8 weeks) and daily oral tenofovir disoproxil fumarate/emtricitabine (TDF/FTC) placebo.
- Arm B – Daily oral TDF/FTC and intramuscular CAB LA placebo injection every 8 weeks.
Results
A total of 38 women in the trial acquired HIV: four from the CAB LA arm and 34 in the FTC/TDF arm. Therefore, the HIV incidence rate was 0.21 percent in the CAB LA group and 1.79 percent in the FTC/TDF participants. The investigators said that while both methods were highly effective at preventing HIV acquisition, CAB LA was 89 percent more effective than FTC/TDF.
Both drugs were well-tolerated with most adverse events being mild or moderate in severity. Injection site reactions were slightly higher in the CAB LA arm and gastrointestinal disorders and nausea were more common in the FTC/TDF arm. There were no discontinuations due to injection site reactions or injection intolerance in either arm of the study.
CAB LA availability
The trail participants, including those in the FTC/TDF arm will have CAB LA will be made available to them, according to reports. Those who do not want to receive CAB LA will be offered FTC/TDF until the originally planned study end date.
Before it can be made more widely available the results of the HPTN 084 study will have to be fully reviewed and submitted for regulatory approval. CAB LA and manufacturing capacity will also have to be developed and further open-label extension studies will be needed to answer some remaining concerns, such as safety in adolescents and pregnant and breastfeeding women.
The World Health Organization (WHO) cautioned that while the results are encouraging, it is also important to temper expectations because of these important safety and implementation issues that need addressing. As a result, the WHO said it is likely to be more than a year before CAB LA will be more widely available.
A similar study (HPTN 083) in HIV-uninfected cisgender men who have sex with men and transgender women who have sex with men, was also stopped early by its DSMB in May 2020, after it also demonstrated that CAB LA was highly effective in preventing HIV acquisition in this group. Final analysis demonstrated the superiority of CAB LA compared to FTC/TDF for PrEP in the HPTN 083 study population.
The WHO continues to recommend oral daily PrEP for the prevention of HIV acquisition in anyone at substantial HIV risk.